The extent of lymphadenectomy in endometrial cancer and its effect on blood loss and procedure duration
Marcin Opławski1, Tomasz Bieda2, Marcin Zarawski1, Zbigniew Kojs2
 Affiliacja i adres do korespondencji
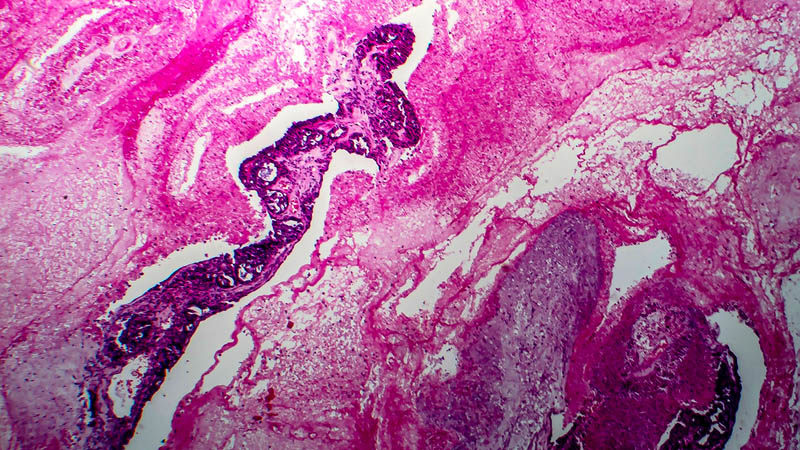
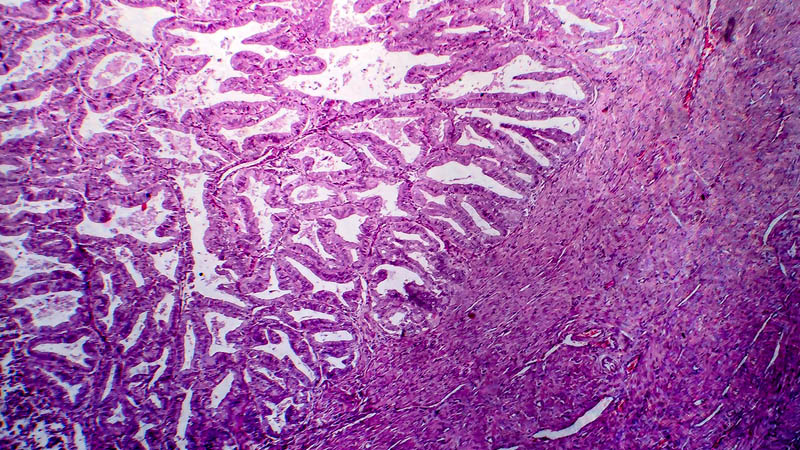
Affiliacja i adres do korespondencjiThe clinical staging of endometrial cancer is performed based on surgical-pathological criteria. The extent of lymph node dissection represents a clinical problem. The study was performed in order to assess the occurrence of metastases in iliac and para-aortic lymph nodes as well as to compare selected surgical risk factors in the case of extending the surgery with the dissection of these lymph nodes. The control group included 27 patients undergoing hysterectomy with iliac lymph node dissection; the study group included 30 patients after iliac and para-aortic lymph node removal. The incidence of metastases was assessed as well as the duration of procedure and intraoperative blood loss were compared. Metastases to lymph nodes were found in 10 (17.5%) females. Iliac lymph node metastases were detected in four patients (14.8%) in group I. In group II, metastases were detected in six (20%) patients: isolated para-aortic metastases in two patients (6.67%), para-aortic and iliac metastases in four (13.33%) patients. Statistically significant difference (p = 0.0035) was found in the duration of procedures: the median was 102.5 minutes for iliac lymphadenectomy, and 132.5 minutes for iliac/para-aortic lymphadenectomy; the maximum duration of iliac/para-aortic lymphadenectomy was 20 minutes longer. There was no statistically significant difference in blood loss (p = 0.4980). However, significantly higher maximum blood loss volume was noticeable in the study group. It is necessary to adjust the para-aortic lymphadenectomy in endometrial cancer to patient’s health status as well as to make maximum use of preoperative diagnostics. The procedure should be performed by a specialist experienced in gynecologic oncology to minimize the surgical risk. Information on lymph node status is the most important prognostic factor in endometrial cancer, which allows for a proper qualification for adjuvant therapy.