Current opinions on possible preservation of fertility in patients undergoing antineoplastic therapy
Jakub Rzepka, Kamil Zalewski, Mariusz Bidziński
 Affiliacja i adres do korespondencji
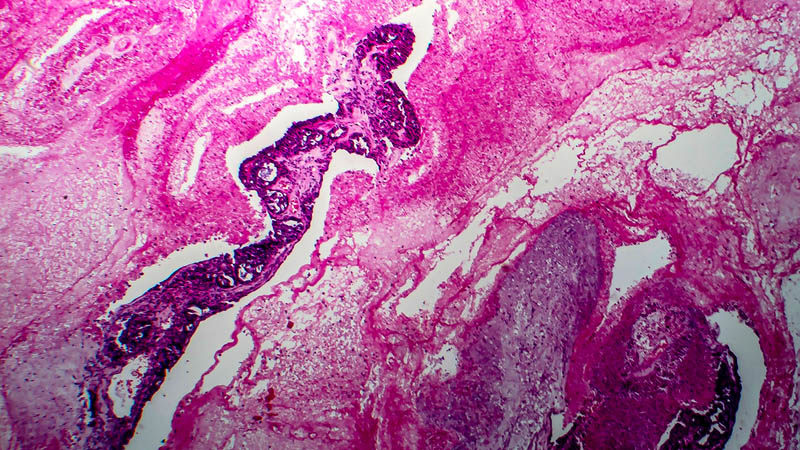
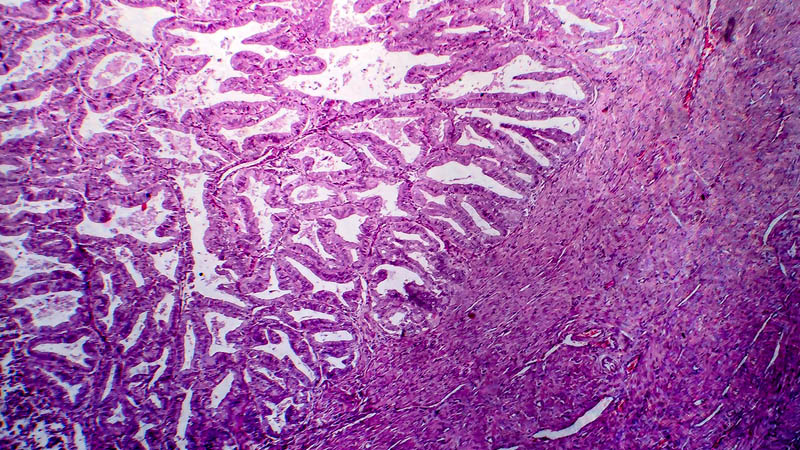
Affiliacja i adres do korespondencjiImplementation of increasingly aggressive protocols in oncology results in increasing permanent cure rates. This is particularly noticeable in the youngest age group, including women of reproductive age. In this population of patients, permanent cure rates may reach 75% according to some authors. Unfortunately, implemented treatment frequently results in a compromised function of gonads and associated therewith secondary infertility, thus significantly influencing the patients’ quality of life. Aggressive and multidrug systemic therapy, used in most frequent paediatric malignancies, e.g. in Hodgkin disease or haematological neoplasms, is associated with high risk of ovarian damage. Particularly gonadotoxic effects have been documented after radiotherapy and alkylating agents-based chemotherapy. At present, there are several methods aiming at preservation of reproductive capacity of patients undergoing such treatment. Currently used transposition of ovaries out of irradiated area and freezing of embryos, in spite of considerable effectiveness, are burdened by several limitations and do not solve the problem of infertility in a satisfactory way, particularly in the youngest oncologic patients. Recently, research is focused on attempts of using GnRH agonists and antagonists, as well as on freezing immature oocytes. Among novel techniques, considerable hopes are associated with freezing and transplantation of ovarian tissue. These procedures do not delay implementation of antineoplastic treatment and do not compromise its effectiveness, but as novel still raise much controversy and debate.