The assessment of some histoclinical factors influencing on lymph node metastasis and risk of recurrences analysis in endometrial cancer patients
Mariusz Bidziński, Anna Dańska-Bidzińska, Grzegorz Panek, Piotr Sobiczewski, Ryszard Krynicki
 Affiliacja i adres do korespondencji
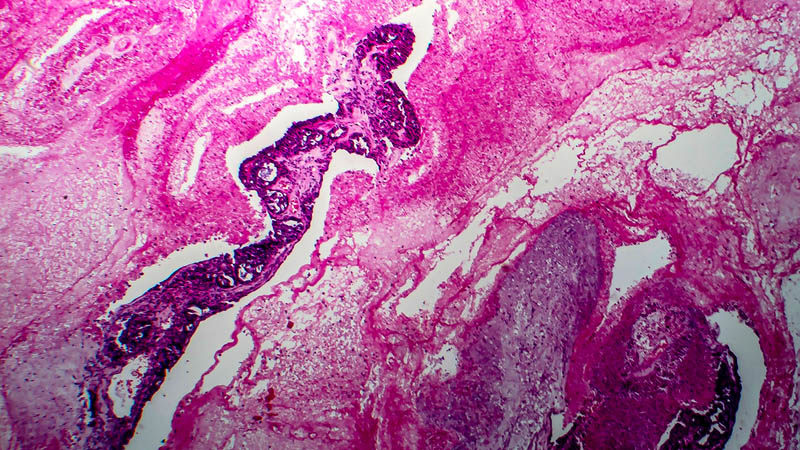
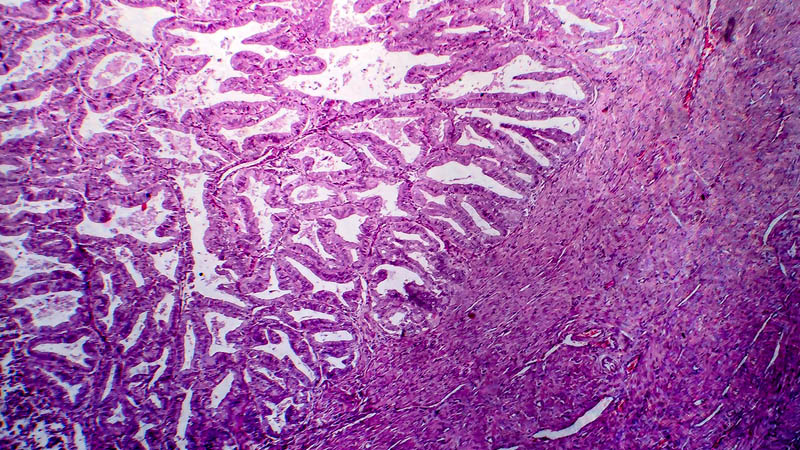
Affiliacja i adres do korespondencjiObjectives: Endometrial cancer is still one of the morbidity leader among women in Poland. The risk of the lymph node involvement depends on some factors i.e.: histological grade, myometrial invasion, histological subtype. Stage IIIC of this cancer, although not very common, makes results of patients treatment unsatisfactory. Design: Taking these facts into consideration the analysis of some histological and clinical factors were assessed in group of patients with endometrial cancer treated in Oncology Center. The subgroup of stage IIIC have been divided, and above mentioned parameters were correlated with time to progression. Material and methods: There were 347 patients selected in to analyzed group. All patients had total hysterectomy with pelvic nodes excision. In some cases with positive pelvic nodes, paraaortic lymphadenectomy were subsequently performed. Age, duration of symptoms, comorbidity, histologic type, grading, and other clinical parameters have been correlated to assess risk of lymph node metastases and time to progression. Results: Tumor diameter, depth of myometrial invasion, histological grade, serous or clear cell carcinoma and spread beyond uterus were main predictive factors of lymph node involvement. It appeared that non-optimal debulking of grossly involved nodes had significant influence on time to progression. Optimal debulking gives, mean 21 months free of disease, comparing with 8 months in patients non-optimally debulked. Serous or clear cell types of cancer, simultaneous involvement of pelvic and paraaortic nodes had also negative prognostic value. Conversely using postoperative radiochemotherapy, time to progression was prolonged. Conclusions: It was noted that lymph node involvement appeared in 13.5% of cases in analyzed group. It should be noted that radiochemotherapy in patients with endometrial cancer stage IIIC is very helpful therapeutic option after complete surgery. Fully excised grossly involved lymph nodes have significant influence on treatment results.